
TALON Help Center
Groups & Eligibility
Confirm that the Client's Employer Groups and Members with Health Insurance Plans are reflected accurately within the TALON Platform. The Client's adjudication engine is considered the Source of Truth.
TALON CSM Role
Orientation on 'Employers' and 'Members' tables within the Support Dashboard.
Client Role
Confirm that all Employers with health insurance Plans, and the Members with health insurance plans within those Employers, are present in the TALON Platform.
Process
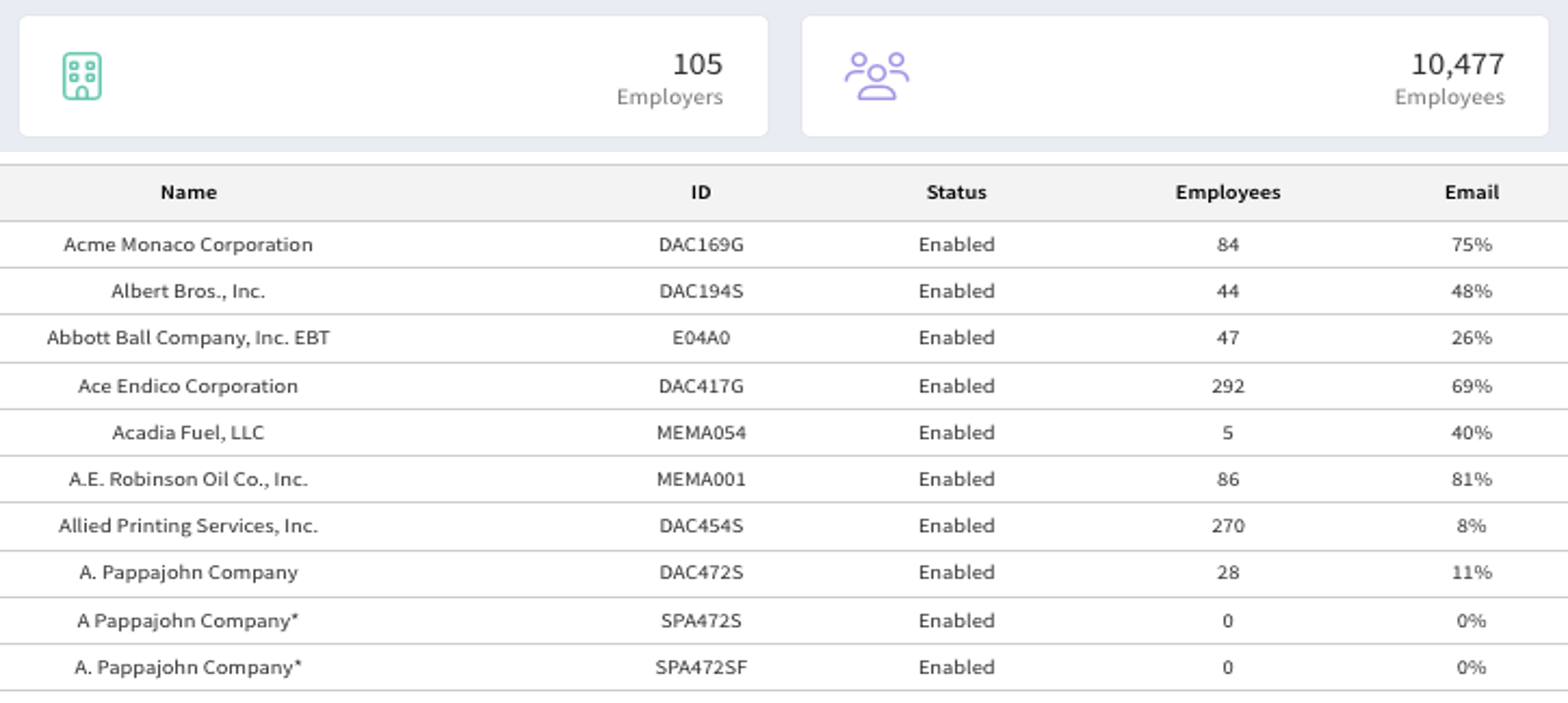
Confirmation Steps
-
Confirm the numbers of Employers and the numbers of Members reflect the expected number in the adjudication engine.
-
Confirm Employee counts within Employers are consistent with the adjudication engine. Look for Employers with 0 Employees.
-
Review Email % and consider creating a remediation plan if needed. Emails are key to Engagement campaigns.
-
Confirm recent Employers added and dropped by Employer Name.
-
Confirm Employer Name to Employer ID are consistent with the adjudication engine. Look for and confirm or resolve null Employer ID's.
-
Confirm recent Members added and dropped by Member Name.